Why Getting This Code Right Matters More Than You Think
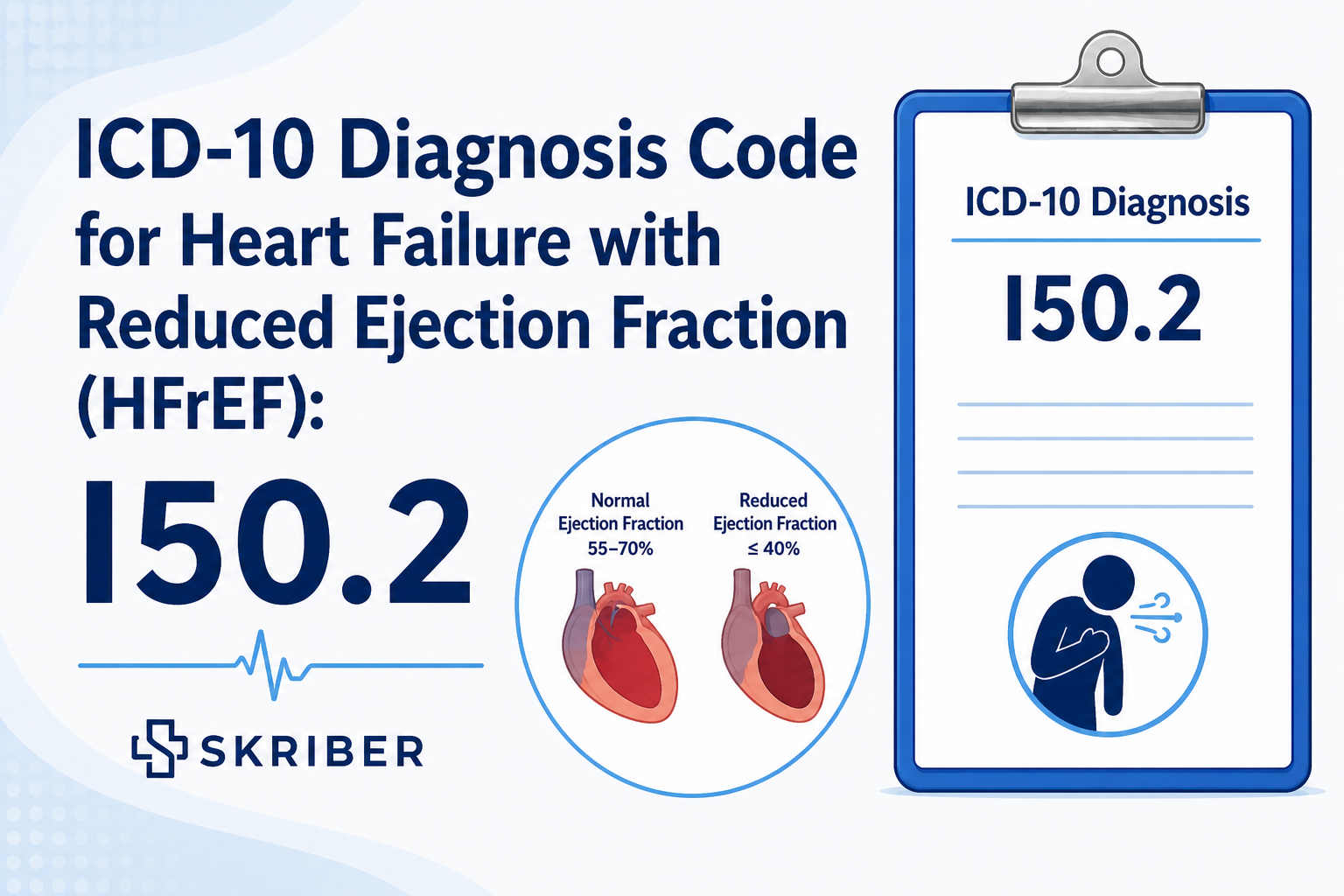
As healthcare professionals, we know that heart failure is not a single disease. It is a complex syndrome with different types. One of the most common types is Heart Failure with Reduced Ejection Fraction, or HFrEF. In this condition, the heart muscle becomes weak. It cannot pump blood well to the rest of the body. The ejection fraction, or EF, is 40% or less. Using the right ICD-10 code for HFrEF is very important. The correct code is I50.2. This code tells the whole story of the patient’s condition. It tells other doctors, nurses, and coders exactly what is happening inside the heart. When you use I50.2, you are saying that the patient has systolic heart failure. This means the “squeeze” of the heart is weak.
Getting this code wrong can cause big problems. The patient’s medical record might not show the true severity of their illness. The hospital or clinic might lose money because of denied claims. Most importantly, the patient might not get the right treatments. Drugs like beta-blockers, ARNIs, and SGLT2 inhibitors are proven to help HFrEF. But these drugs work best when the diagnosis is clearly coded as I50.2.
What Exactly is HFrEF?
Let us break down the term HFrEF. HF stands for heart failure. This means the heart is not meeting the body’s needs. rEF stands for reduced ejection fraction. Ejection fraction is a simple number. It is the percent of blood the left ventricle pumps out with each beat. A normal heart pumps out 50% to 70% of the blood inside it. In HFrEF, that number drops to 40% or less.
Think of the heart like a rubber ball. A healthy heart squeezes hard and pushes most of the blood out. A heart with HFrEF is like a wet, weak sponge. It still squeezes, but very little blood comes out. The rest of the blood stays inside the heart. This extra blood backs up into the lungs and body. The patient feels short of breath. Their legs may swell. They feel tired all the time.
Doctors find HFrEF using a simple test called an echocardiogram, or echo. The echo measures the ejection fraction directly. An EF of 40% or less confirms HFrEF. An EF of 41% to 49% is called HFmrEF (heart failure with mildly reduced ejection fraction). An EF of 50% or more is called HFpEF (heart failure with preserved ejection fraction). Only I50.2 is for the reduced type below 40%.
| Condition | Ejection Fraction (EF) | Correct ICD-10 Code |
|---|---|---|
| Normal Heart Function | 50% – 70% | No heart failure code |
| HFrEF (Reduced) | 40% or less | I50.2 |
| HFmrEF (Mildly Reduced) | 41% – 49% | I50.9 (Heart failure, unspecified) |
| HFpEF (Preserved) | 50% or higher | I50.3 (Heart failure with preserved EF) |
Breaking Down the ICD-10 Code I50.2: Systolic (Congestive) Heart Failure
The full official name for code I50.2 is “Systolic (congestive) heart failure.” You may also see it written as “Heart failure with reduced ejection fraction” or “HFrEF.” All of these names mean the same thing. The word “systolic” refers to the squeezing phase of the heartbeat. So systolic heart failure means the squeeze is weak.
This code lives inside the larger ICD-10 chapter for diseases of the circulatory system (I00-I99). More specifically, it is under I50, which is for heart failure. The I50.2 code has a few sub-codes that give more detail. You must know these sub-codes to code correctly. Using only I50.2 without a fourth or fifth character is not complete.
Here are the important sub-codes under I50.2:
- I50.20: Systolic (congestive) heart failure, unspecified. Use this when the note says “HFrEF” but does not say if it is acute or chronic.
- I50.21: Acute systolic (congestive) heart failure. Use this for a new, sudden, or worsening case. The patient is having symptoms right now, often needing hospital care.
- I50.22: Chronic systolic (congestive) heart failure. Use this for a long-term, stable case. The patient has known HFrEF but is not in a sudden flare-up.
- I50.23: Acute on chronic systolic (congestive) heart failure. Use this when a patient with chronic HFrEF has a sudden worsening. They were stable, but now they are having an acute flare-up. This is very common in hospital admissions.
Choosing between I50.21, I50.22, or I50.23 changes the severity of the diagnosis. It also changes the expected level of care. Always read the doctor’s note carefully to find the words “acute,” “chronic,” or “acute on chronic.”
How to Document HFrEF for Accurate Coding: A Practical Guide
Documentation is the bridge between the patient and the code. If you do not write it down, it did not happen. The coding team cannot guess what you mean. You must write clear, simple words. For HFrEF, you should always include the ejection fraction number. Write “EF 35%” or “ejection fraction 30%.” This number is the best proof that the patient truly has HFrEF.
You also need to document the timing of the condition. Use one of these three phrases exactly:
- “Acute systolic heart failure” (for sudden or new cases)
- “Chronic systolic heart failure” (for stable, long-term cases)
- “Acute on chronic systolic heart failure” (for a sudden flare-up of a chronic problem)
Do not just write “CHF” or “heart failure.” These terms are too vague. They could mean HFrEF, HFpEF, or something else. In fact, the ICD-10 guidelines say you should not code HFrEF from the term “CHF” alone. The note must say “systolic” or “reduced ejection fraction.” Otherwise, the coder must use the unspecified code I50.9.
Checklist for Good HFrEF Documentation:
- Write “HFrEF” or “systolic heart failure”
- Include the EF number (e.g., EF 25%)
- State the timing: acute, chronic, or acute on chronic
- List the symptoms (dyspnea, edema, fatigue)
- Mention the treatments (diuretics, beta-blockers, etc.)
Common Mistakes to Avoid When Using I50.2
Even experienced clinicians make coding mistakes. The most common error is using I50.9 (heart failure, unspecified) when you really mean I50.2. Why does this happen? Sometimes doctors write “CHF” and nothing else. The coder has no proof of reduced EF. So they must use the unspecified code. This is a lost opportunity. Unspecified codes do not reflect the true diagnosis. They also pay less than specific codes.
Another common mistake is mixing up acute and chronic. For example, a patient comes to the ER with sudden shortness of breath. They have a known history of HFrEF. The attending doctor writes “chronic HFrEF” in the note. But the patient is in an acute flare-up. The correct code should be I50.23 (acute on chronic). The wrong code (I50.22 for chronic) under-states the severity. This can lead to a shorter hospital stay or a denied claim.
A third mistake is forgetting to code the cause of HFrEF. I50.2 tells us the patient has weak heart pumping. But it does not tell us why the heart is weak. Common causes include ischemic heart disease (old heart attacks), high blood pressure, or valve problems. You should code these causes as separate diagnoses. For example, code I25.10 for atherosclerotic heart disease. Code I10 for hypertension. This gives a full picture of the patient.
| Mistake | Example | How to Fix It |
|---|---|---|
| Using I50.9 for HFrEF | Doctor writes “CHF” but means HFrEF | Always write “systolic” or “reduced EF” |
| Wrong timing code | Patient has acute worsening, but note says “chronic” | Document “acute on chronic” when appropriate |
| Missing the cause | Only code I50.2, ignore the heart disease | Add codes for CAD, HTN, or valve disease |
Other Heart Failure Codes You Need to Know (I50.1, I50.3, I50.4, I50.9)
It is helpful to see how I50.2 fits with the other heart failure codes. This will keep you from using the wrong one. Here is a simple guide to the most common I50 codes.
I50.1 – Left ventricular failure (LVF). This is a tricky code. It is often used for acute pulmonary edema. But official guidelines say I50.1 is not the same as I50.2. In fact, I50.2 (HFrEF) is the preferred code for chronic systolic failure. Use I50.1 only for specific cases of left ventricular failure without the term “systolic” or “HFrEF.”
I50.3 – Heart failure with preserved ejection fraction (HFpEF). This is the opposite of HFrEF. In HFpEF, the ejection fraction is normal (50% or more). The heart squeezes fine, but it is too stiff to relax and fill with blood. This is diastolic heart failure. Do not use I50.2 for these patients. Use I50.3 instead. The treatments are different, so the code must be different.
I50.4 – Combined systolic and diastolic heart failure. This code is for patients who have both problems. Their EF is reduced (systolic failure) and their heart is stiff (diastolic failure). Some doctors call this “mixed heart failure.” Use this code only when the note clearly says both types are present.
AI-Powered • HIPAA-Ready
Let AI handle your clinical notes.
Skriber listens during the visit and creates complete SOAP notes in seconds — so you can stay focused on the patient.
-
Capture Ambient listening during sessions
-
Transcribe Speech → text instantly
-
Generate SOAP Accurate structured notes
-
Review & sign Edit and finalize instantly
I50.9 – Heart failure, unspecified. This is your last resort. Use it only when the note says “heart failure” or “CHF” with no other details. Do not use it if you know the EF is reduced. I50.9 should be less than 10% of your heart failure codes in a good documentation system.
How I50.2 Affects Treatment, Billing, and Reimbursement
Codes are not just for statistics. They directly affect patient care and money. When you use I50.2, you are telling the healthcare system that this patient needs certain proven treatments. For HFrEF, the guidelines recommend four main drug classes. These are called “Guideline-Directed Medical Therapy” or GDMT. They include beta-blockers, ACE inhibitors or ARBs, ARNIs (like sacubitril/valsartan), and SGLT2 inhibitors (like dapagliflozin). If the code is I50.2, the computer system will flag if these drugs are not ordered.
The code also affects billing and reimbursement. Medicare and private insurance companies look at diagnosis codes to decide how much to pay. A specific code like I50.21 (acute systolic heart failure) pays more than an unspecified code like I50.9. Why? Because acute heart failure is more serious. It requires more nursing time, more tests, and more intensive treatments. The higher payment matches the higher work.
Hospitals also use these codes for quality reporting. For example, the “Hospital Readmission Reduction Program” tracks how many heart failure patients come back within 30 days. But the program specifically looks at patients coded with I50.2, I50.3, and I50.4. If you use I50.9 too often, the hospital’s data becomes inaccurate. This can lead to financial penalties from Medicare. So using I50.2 correctly is not just good medicine. It is good business.
Case Examples:
Let us walk through three patient cases. These examples show how to choose the right code for HFrEF. Read each case and think about the correct I50.2 sub-code.
Case 1: New Diagnosis in Clinic
A 62-year-old man comes to your office for a routine visit. He has been feeling more tired over the last three months. He gets short of breath when he walks up one flight of stairs. An echo shows an ejection fraction of 35%. He has never had heart failure symptoms before today. His condition is stable enough to go home with new medicines.
Correct code: I50.22 (Chronic systolic heart failure). Even though this is a new diagnosis, it is not acute. The patient is stable and does not need the hospital.
Case 2: Emergency Admission
A 78-year-old woman with known HFrEF (EF 30%) comes to the ER. She cannot breathe while lying flat. She has crackles in both lungs. Her legs have new swelling. She was fine yesterday. Today she is very sick. The doctor admits her to the hospital.
Correct code: I50.23 (Acute on chronic systolic heart failure). She has chronic HFrEF, but now she has a sudden worsening.
Case 3: First Heart Attack
A 55-year-old man has a large heart attack (STEMI). He is admitted to the ICU. An echo the next day shows his EF has dropped from 55% to 40%. He is short of breath and needs oxygen. The heart attack is new, and the heart failure is new.
Correct code: I50.21 (Acute systolic heart failure). This is a new, sudden case. There is no prior history of chronic HFrEF.
Final Summary and Quick Reference
Coding heart failure correctly is a skill. It requires clear thinking and clear writing. For HFrEF, always remember the number 40. If the ejection fraction is 40% or less, you are in I50.2 territory. Then ask yourself one more question: Is this acute, chronic, or acute on chronic? Write that word in your note. Your coders will thank you. Your billing department will thank you. Most of all, your patients will get the right care.
Here is a quick reference card you can save or print.
Quick Reference: ICD-10 Code I50.2 for HFrEF
- Definition: Systolic heart failure with EF ≤ 40%
- Main Code: I50.2 (Systolic congestive heart failure)
- Sub-codes:
- I50.20 = Unspecified (use only if timing is unknown)
- I50.21 = Acute (new or sudden onset)
- I50.22 = Chronic (stable, long-term)
- I50.23 = Acute on chronic (worsening of stable HFrEF)
- Do NOT use I50.2 for: HFpEF (EF ≥ 50%) or unclear cases (use I50.9 instead)
- Documentation must include: The phrase “systolic” or “reduced EF,” the EF number, and the timing (acute/chronic)
- Always code the cause: Add codes for ischemic heart disease (I25.10), hypertension (I10), or valve disease (I34-I37)
The bottom line is simple. Specific codes lead to specific care. And specific care saves lives. Next time you see a patient with heart failure, ask for the ejection fraction. Then use the power of I50.2 to tell the whole story. Your precision as a healthcare professional starts with the words you write and the codes you choose. Make every code count.
for clinicians · HIPAA-ready
Spend more time with patients, not paperwork.
Skriber transforms ambient speech into accurate SOAP notes — finished before your next session.
No credit card required.

Dr. Connor Yost is an Internal Medicine resident at Creighton University School of Medicine in Arizona and an emerging leader in clinical innovation. He currently serves as Chief Medical Officer at Skriber, where he helps shape AI-powered tools that streamline clinical documentation and support physicians in delivering higher-quality care. Dr. Yost also works as a Strategic Advisor at Doc2Doc, lending his expertise to initiatives that improve financial wellness for physicians and trainees.
His professional interests include medical education, workflow redesign, and the responsible use of AI in healthcare. Dr. Yost is committed to building systems that allow clinicians to spend more time with patients and less on administrative tasks. Outside of medicine, he enjoys photography, entrepreneurship, and family life.